(Toxic Epidermal Necrolysis, Stevens-Johnson syndrome, Fiessinger-Rendu erosive pluriorificial ectodermosis)
Very rare: about 1/500.000/year. Acute onset destruction of the superficial layer of the skin and mucous membranes.
There are different presentationsĀ:
- Stevens-Johnson syndrome: < 10% of the skin surface is peeled off or removable
- Lyell syndrome: > 30%
- overlap syndrome: between 10 and 29%
- severe form of graft-versus-host disease after bone marrow transplantation
Causes:
- in 70% of cases, it is a kind of drug allergy: anti-infective sulfonamides, allopurinol, carbamazepine, phenytoin, phenobarbital, lamotrigine, NSAIDs oxicams, nevirapine (anti-HIV) derivatives. The delay between the introduction of the drug and the first clinical signs ranged from 4 to 28 days. Genetic predisposition: group HLA-B*5801 for the form induced by allopurinol and HLAB*1502 for the form induced by carbamazepine (Chinese populations) (6p21.33)
- in 10% of cases: idiopathic
- in 20%: other causes like AIDS, pneumonia, Mycoplasma pneumoniae
Clinical presentation:
- onset with fever and a skin rash (face, trunk) spreading in a few hours or days
- the mucosae are affected in 90% of cases, preceding the skin lesions by 1 to 3 days (30%): all orifices can be involved.
- cutaneous target-like lesions with a darker middle: evolution from macules to papules to blisters to purpuric plates and finally skin shedding following minor trauma (Nikolski sign)
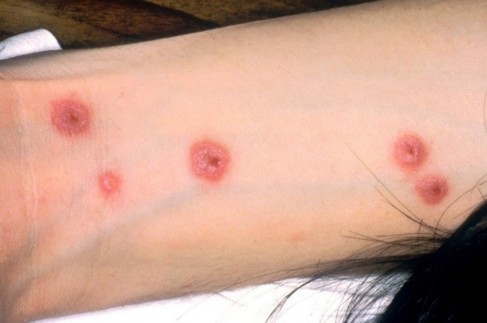
- involvement of the digestive tract: colitis
- hepatitis: 10%
- ARDS in case of involvement of the respiratory mucosa (20 %)
Significant mortality linked to the % of affected skin surface.
Anesthetic implications:
* protect the affected areas
* vascular access in healthy zone for rehydration and analgesia
* prevention of hypothermia
* asepsis
* transfer to a specialized centre (burn center)
- anesthesia: asepsis, echocardiography and chest XRay, liver function, difficult control of the upper airway if non-intubated
References :
- He M.
Emergent retrograde tracheal intubation in a 3-year-old with Stevens-Johnson syndrome.
A&A Case Reports; 2014: 2: 7-8
- contact.bulle@hmn.aphp.fr
- Roujeau J-C.
Syndroles de Lyell et de Stevens-Johnson.
Encyclopédie Orphanet juin 2007
Updated: June 2019