(Adenocutaneomucous syndrome)
More frequent in children of Asian (incidence of 240/100.000 less than 5 years old children versus 4-25/100.000 in Europa and in the U.S.A.) or Afro-Caribean origin. Multisystemic febrile vasculitis of unknown etiology: fever, conjunctivitis, polymorphous rash, vasculitis, coronary aneurysms. It is the most common cause of acquired cardiac pathology in children in developed countries. This vasculitis mainly affects children under 5 years of age (80 %) (peak 9-11 months-old infant) and involves the medium size arteries (coronary, mesenteric, iliac). The cause is probably an unknown infectious agent that causes a particular immune response (increase of circulating B lymphocytes) in genetically predisposed individuals. In the absence of treatment, aneurysms of the coronary arteries develop in 18-23 % of the cases (and in less than 5 % in case of early treatment) and there is a risk of death from myocarditis, LV dysfunction or myocardial infarction. There are other complications and modes of presentation: aseptic meningitis, pneumonia with pleural effusion, cholecystitis, pancreatitis, myositis, pericarditis.
In the absence of diagnostic test, the diagnosis is clinical:
Diagnostic criteria of Kawasaki disease
|
1 |
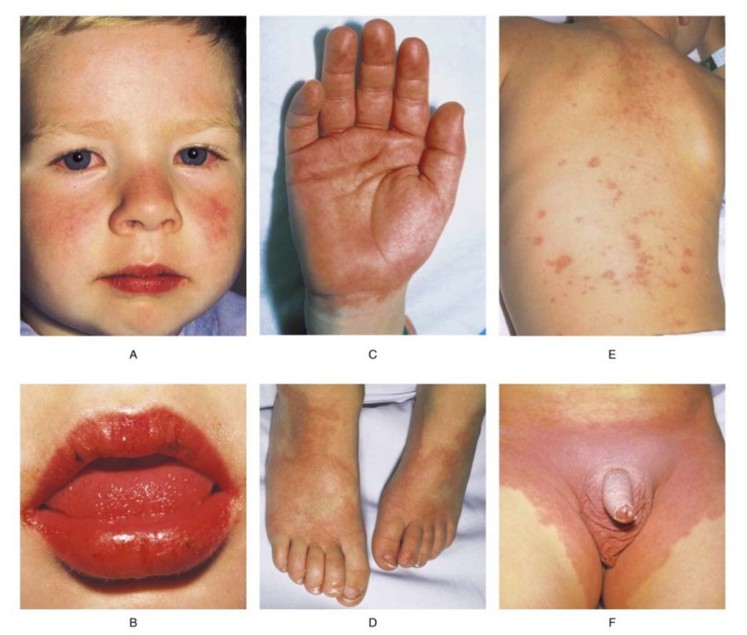
bilateral non-exsudative conjonctival injection (a) |
|
2 |
cervical adenopathy: at least 1 ganglion with a diameter >1,5 cm |
|
3 |
diffuse, morbilliform or scarlatiniform maculopapulous rash on the trunk and limbs, typical perineal localization (e, f) |
|
4 |
oropharyngeal involvement: cheilitis, stomatitis, raspberry tongue (b) |
|
5 |
involvement of feet and hands: edema, induration, desquamation (c, d) |
Two types of Kawasaki disease are distinguished:
- classic or typical kawasaki if fever since ≥ 5 days and ≥ 4 of the 5 criterias,
or if fever since ≥ 5 days and ≥ 4 of the 5 criterias + coronary aneurysms
- incomplete or atypical kawasaki if fever since ≥ 5 days and ≥ 2 of the 5 criterias
The patients with an incomplete form have an increased risk of developping coronary aneurysms as the diagnosis is delayed, or even missed.
|
Main
|
Liver
|
High band
|
Cervical
|
Young
|
|
age |
older |
intermediate |
intermediate |
younger |
|
Adenopathies
|
intermediate |
low |
high |
low |
|
|
SGPT, ăGT and high total bilirubin , high hemoglobin |
immature ++ neutrophils but lowest white blood cells and platelets count |
high white blood cells and platelets ; very high CRP;
|
highest
|
|
Risk of
|
|
|
|
|
|
resistance to gammaglobulins |
high |
intermediate |
intermediate |
low |
|
Incidence
|
low |
high |
intermediate |
low |
Echographic criterias of the coronary involvement:
|
* Z-score of the anterior interventricular (IVA) or the right coronary artery (ACD) ≥ 2.5 * presence of a coronary aneurysm * ≥ 3 of the next criterias: - decreased systolic function of the left ventricle - mitral regurgitation - pericardial effusion - and/or Z-score of the IVA and the ACD between 2-2.5 |
Classification of the coronary involvement according to the Z-score:
|
degree of coronary involvement |
coronary diameter (Z-score ± absolute dimension) |
|
1. no involvement |
- always < 2 |
|
2. dilation alone |
- 2 to < 2.5; or initially < 2, diminution of Z-score of more than 1 during the follow-up |
|
3. small size aneurysm |
- > 2.5 to 5 |
|
4. medium size aneurysm |
- > 5 to < 10 and absolute dimension < 8 mm |
|
5. large size or giant aneurysm |
- > 10 or absolute dimension > 8 mm |
During the acute phase of the disease, the child can present with two more severe forms:
- either a sort of cardiogenic shock (KDSS for Kawasaki Disease Shock Syndrome) : arterial hypotension with or without vasoconstriction, resistant to treatment and associated with echocardiographic (LV dysfunction, mitral regurgitation, pericardial effusion) and biologic signs of myocarditis (tropinin) or cardiac failure (proBNP).
- or a form of activation of the macrophages (MAS Macrophage Activation Syndrome). It is a form of lymphohistiocytic hemophagocytosis of viral origin with a cytokinic storm (see this term).
A syndrome quite similar to Kawasaki disease (or PIMS, acronym for Pediatric Multisystem Inflammatory Syndrome) (see this term) has been observed during the COVID-19 pandemic: it involved children generally older than 5 years old in a typical context of fever during several days with diarrhea and abdominal pain, evolving into a hyperinflammatory state (cytokinic storm), intermediate between Kawasaki disease and toxinic shock. Most of those children had been infected by the COVID-19 and all have responded favorably to administration of IV immunoglobins and corticosteroids.
The spontaneous evolution of the classical form of the Kawasaki disease progresses in 3 successive stages:
- acute phase (from 1st to 7-14th day): fever resistant to antibiotics. The cardiac involvement may present as a partial AVB, disorders of repolarization (flattened T wave), LV and RV hypokinesia, pericardial effusion, dilation of the coronary arteries ...
- subacute phase (from the 10th to the 25th day): fever often disappears and the extremities are desquamating. Arterial aneurysms, including coronary ones, are present in 20 % of cases. Major thrombocytosis is present with a risk of thrombosis and ischemia. The diagnosis is not easy to establish during these two periods because the signs of the disease are not always simultaneously present at the same time; in addition, the presentation can be atypical: meningitis or aseptic arthritis for example.
- convalescence (6 to 8 weeks after the onset): in the absence of treatment, the vascular lesions spontaneously evolves towards thrombosis with myocardial infarction, rupture of pillars, angina. Angina is often silent (clinical manifestations are difficult to interpret in the small child) and the ECG is not very specific .
The algorithm of management recommended by the AHA is
.jpg)
The currently recommended treatment is based on early diagnosis and specialized follow-up:
- acute phase:
o aspirin 80-100 mg/kg in 4 doses up to when fever disappears ; thereafter 2-5 mg/kg/day for at least 6 weeks
o human gammaglobulins: 2 g/kg IV in a single dose if CRP level is > 30 mg/L
o ECG monitoring and echocardiography
- after defervescence (48 h), repeat echocardiography at 2 and 6 weeks and depending on the result:
1) in the absence of coronary aneurysms: aspirin at low doses for up to 6 weeks
2) in case of coronary aneurysms of < 6 mm diameter, without strictures: repeat ultrasound every 6 months and continue aspirin until recession of aneurysms
3) in case of coronary aneurysms of > 6 mm diameter, or stenoses: continue aspirin and consider adding an antithrombotic treatment with vitamin K antagonists; continue aspirin and associate atheromatosis prophylaxis; repeat ultrasound every 6 months (possibly coronary angiography and stress test)
- in the absence of defervescence after 48 h or in case of relapse within 2 weeks (in 20 % of the cases): repeat a dose of IV gammaglobulin and add corticosteroids (methylprednisolone 30 mg/kg/d). Infliximab (5 mg/kg in one IV dose) is used in case of absence of response to corticotherapy or in case of very severe form.
Children with giant coronary aneurysms (z-score ≥ 10 or diameter ≥ 8 mm) have a high risk of serious cardiovascular events including STEMI or non-STEMI-type myocardial infarctions. Management is similar to that in adults: emergency coronography, most often with fibrinolysis.
Short summary:
STEMI (severe ischemia and myocardial necrosis)
♦ access to cardiac catheterization < 90 minutes after first medical contact
1) clopidogrel orally: 0.2 mg/kg if infant, 1 mg/kg if child; prasugrel 60 mg if adolescent
2) IV heparin as soon as venous access is obtained: 75 IU/kg followed by 20 IU/kg/h
3) if large thrombus: aspiration is not recommended but consider an IIb/IIIa platelet receptor antagonist: eptifibitide 180µg/kg then 2µg/kg/h for 12 hours
♦ access to cardiac catheterization > 90 minutes after first medical contact
1) pending transfer to the catheterization room: tissue plasminogen activator (tPA): 0.03 to 0.1 mg/kg/h for 6-12h, max 2 mg/h; beware that the fibrinogen level must be > 150 mg/dl: otherwise 10-20 ml/kg of PFC should be administered
2) start IV heparin 10 U/kg/h via a different IV line than tPA, and continue for 6 hours after stopping the tPA.
3) coronarography as soon as possible
♦ no access to cardiac catheterization
1) start treatment with tissue plasminogen activator (tPA): 0.03 to 0.1 mg/kg/h for 6-12h, max 2 mg/h; beware that the fibrinogen level must be > 150 mg/dL, otherwise 10-20 ml/kg of PFC should be administered
2) start IV heparin 10 U/kg/h via a different IV line than tPA;
3) check the level of antithrombin III and adjust to obtain a blood level of 80 at 120 %
4) at the end of the tPA infusion, adjust the heparin dose to get an activated clotting time of 200-250 sec
4) to inhibit platelet aggregation: consider an IIb/IIIa platelet receptor antagonist: eptifibitide 180 µg/kg and then 2 µg/kg/h for 12 hours (adult data)
5) in case of chest pain: administer a nitro derivative sublingually or IV; watch out for the risk of hypotension
Non-STEMI (insufficient input of O2 to the myocardium without necrosis): ECG abnormalities and increased troponin level:
1) start IV heparin IV: 75 IU/kg then 20 U/kg/h depending according to the antiXa level
2) start or continue aspirin and start clopidogrel orally: loading dose 2-3 mg/kg followed by 1 mg/kg/d (max 75 mg)
3) perform coronary imaging (CT or coronography)
Anesthetic implications:
in case of coronary artery disease, check myocardial function with a preoperative echocardiography. Monitoring: ECG 5 derivations. Keep this diagnosis in mind in case of a fever in a child less than 5 years old, with a rash and/or lymph nodes or in case of unexpected perioperative cardiac problem (risky situation: negative laparotomy for suspicion of appendicitis).
References :
- Morrison JE, Anderson M, Chan KC, Pietra B, Zuk J, Gnadinger P.
A 15-year review of children with Kawasaki’s syndrome having general anesthesia or sedation.
Pediatr Anesth 2005; 15: 1053-8.
- Bressieux-Degueldre S, Schaffner D, Hofer M, Sekarski N, Vanoni F.
Maladie de Kawasaki : mise ŕ jour.
Revue Médicale Suisse 2018 ; 14 : 384-9
- McCrindle BW, Rowley AH, Newburger JW, et al.
Diagnosis, treatment, and long-term management of Kawasaki disease: a scientific statement for health professionals from the American Heart Association.
Circulation 2017; 135: e927–99.
- Riphagen S, Gomez J, Gonzalez-Martinez C, Wilkinson N, Theocharis P.
Hyperinflammatory shock in children during COVID-19 pandemic.
The Lancet doi.org/10.1016/S0140-6736(20)31094-1 (May 6, 2020)
- Verdoni L, Mazza A, Gervasoni A, Martelli L, Ruggeri M, Ciuffreda M, Bonanomi E, D’Antiga L.
An outbreak of severe Kawasaki-like disease at the Italian epicentre of the SARS-CoV-2 epidemic: an observational cohort study.
The Lancet doi.org/10.1016/S0140-6736(20)31103-X (May 13, 2020)
- Burns JC, El-Said H, Tremoulet AH, Friedman K, Gordon JB, Newburger JW.
Management of myocardial infarction in children with giant coronary artery aneurysms after Kawasaki disease.
J Pediatr 2020 ; 120 : 230-4.
- Wang H, Shimizu C, Bainto E, Hamilton S, Jackson HR, Estrada-Rivadeneyra D, Kaforou M et al.
Subgroups of children with Kawasaki disease: a data-driven cluster analysis.
Lancet Child Adolesc Health 2023; 7: 697–707.
Updated: September 2023