[MIM 231 300, 600 975, 613 085, 613 086, 617 272]
(Buphtalmos)Often sporadic but autosomal recessive transmission in case of mutation of GLC3A/CYP1B1 gene (on 2p) or, more rarely, of FKHL7 gene (on 6p25). Often bilateral (may be unilateral), sometimes asymmetrical, it is due to an anomaly of the iridocorneal angle, in general by persistence of an embryonic membrane (Barkan membrane). Glaucoma is said "primary" if it is caused by an isolated anomaly of development of the iridocorneal angle. It is secondary when it is associated with other ocular or systemic problems (craniofacial malformations, various trisomies and polymalformative syndromes). "Infantile glaucoma" occurs before the age of 3 years, and "juvenile glaucoma" appears later. The clinical signs of congenital glaucoma can be present during the first week of life
- photophobia ;
- clear watery eyes ;
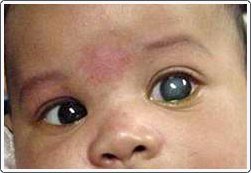
- megalocornea, corresponding to an increased corneal diameter, due to increased intraocular pressure: the eye of the newborn deforms, which can lead to buphtalmos ("Bull's eye" appearance).
The diagnosis will be confirmed bye a ophthalmic examination under general anesthesia, a high IOP (> 21 mmHg) and an enlarged corneal diameter (> 12 mm).
Many syndromes or diseases are associated with congenital glaucoma (see these terms):
- Axenfeld-Rieger
- Peters
- Meckel
- Marfan
- Weil-Marchesani
- homocystinuria
- von Recklinghausen type 1
- Sturge-Weber-Krabbe
- Leber-Coats
- Lowe
- SHORT
- Marshall
- Stickler
- Lowry-Mac Lean
- Melnick-Needles
- oculo-facio-cardio-dental syndrome
Treatments: beta-blockers (eye drops), goniotomy, perforating or external trabeculotomy, trabeculectomy, with valve drainage, laser on the iridocorneal angle
Anesthetic implications:
avoid any compression of the eyeballs with the edges of the face mask. Sevoflurane can be used for induction and maintenance of anesthesia provided high concentrations are avoided: their hemodynamic effects can lead to a decreased intraocular pressure. Laryngoscopy and endotracheal intubation, especially in an incompletely paralyzed child, increase intraocular pressure while insertion of a laryngeal mask has little effect; to ensure accuracy of the results, it is better to measures IOP before the insertion of the laryngeal mask or laryngoscopy.
Beware: in an anesthetized child, the passage from supine to ventral decubitus increases IOP by an average of 7 mmHg and the IOP increases by Ý 2.2 mmHg hourly.
References :
- Geeraerts T, Devys JM, Berges O, Dureau P, Plaud B.
Sevoflurane effects on retrobulbar arteries blood flow in children.
Br J Anaesth 2005; 94:636-41.
- Gulati M, Mohta M, Ahuja S, Gupta VP.
Comparison of laryngeal mask airway with tracheal tube for ophthalmic surgery in paediatric patients.
Anaesth Intensive Care 2004; 32:383-9.
- Watts P, Lim MK, Gandhewar R, Mukherjee A, Wintle R, Armstrong T, Zatman T, Jones R, Al Madfai H.
The effect of laryngeal mask airway insertion on intraocular pressure measurement in children receiving general anesthesia.
Am J Ophthalmol 2007; 144:507-10
- Szmuk P, Steiner JW, Pop RB, You J, Weakley DR, Swift DM, Sessler DI.
Intraocular pressure in pediatric patients during prone surgery.
Anesth Analg 2013 ; 116 : 1309-13
Updated: May 2017